What is Neuropathic Pain?
Neuropathic pain also known as nerve pain is a group of chronic pain conditions caused by a lesion or disease of the somatosensory nervous system. Epidemiological studies have found a prevalence of Neuropathic Pain in about 7-10% of the population and over 20-25% of patients with chronic pain have neuropathic pain characteristics.
Why neuropathic pain happens?
Nerve pain or neuropathy can happen from various reasons. Common neuropathic pain syndromes include painful polyneuropathy (e.g., due to diabetes), postherpetic neuralgia, peripheral nerve injury, radiculopathy, cancer-related pain, central post-stroke pain and trauma- or entrapment neuropathy or postsurgical neuropathy. Neuropathic pain often has a negative impact on the mental health and quality of life in these groups of patients.
How is neuropathic pain different from joint or back pain?
Neuropathic pain typically manifests as tingling, stabbing, burning, electric shock-type, pins needles or increased sensation over the affected nerve and surrounding area.
Treatment of Neuropathic Pain
Neuropathic Pain management is traditionally done by pharmacotherapy and the main focus is on treating symptoms. Typically gabapentinoids, tricyclic antidepressants (TCAs), and selective serotonin–norepinephrine reuptake inhibitors (SNRI) as the first-line drugs for neuropathic pain. Lidocaine, Capsaicin, and Tramadol have been proposed as the second-line treatment, while strong opioids (Morphine and Oxycodone) and botulinum toxin-A (BTX-A) were included as third-line treatments for peripheral neuropathic pain.
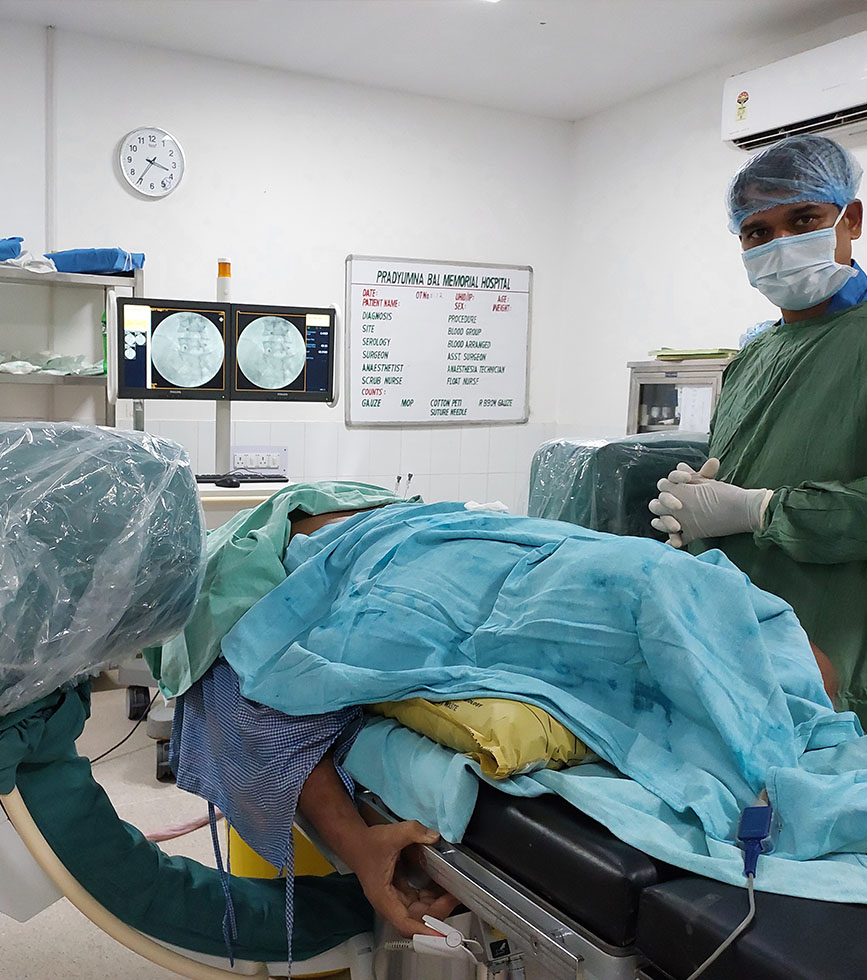
In recent times, interventional pain management like pulsed radiofrequency, cryoneurolysis, peripheral neurostimulation (PNS) or spinal cord stimulation (SCS) seem to be promising. Furthermore, another new minimally-invasive ultrasound guided hydrodissection technique has shown significant improvement in entrapment neuropathies like carpal tunnel syndrome and similar conditions.

